NICU Nurses Adapt for Unique Needs of Twins JamieLynn and AmieLynn Prior to Separation
Twins AmieLynn and JamieLynn Finley won the hearts of the nurses who fed, diapered and bathed the girls a little differently from other babies in the Cook Children’s NICU.
By Jean Yaeger
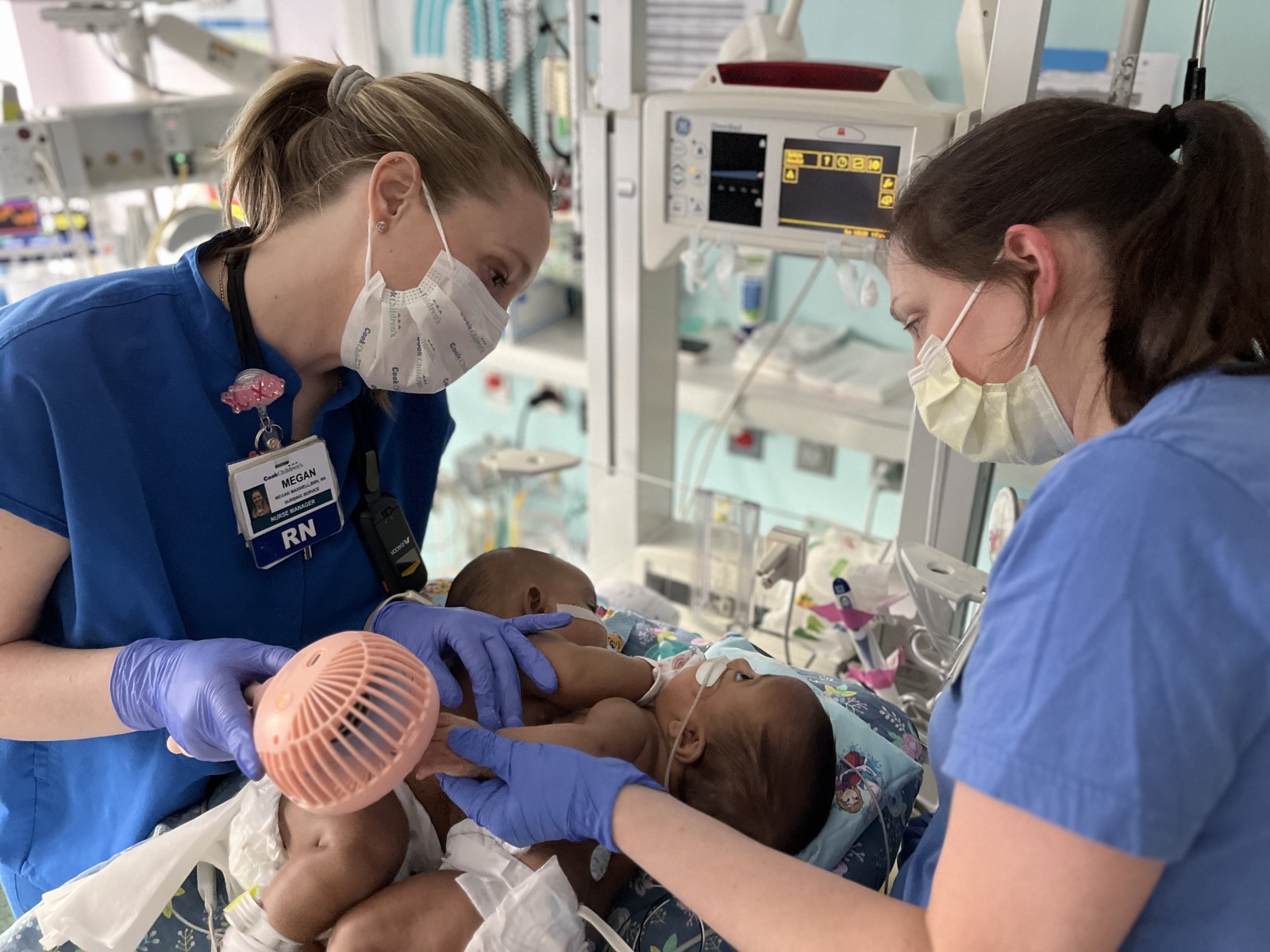 Twins AmieLynn and JamieLynn Finley won the hearts of the nurses who fed, diapered and bathed the girls a little differently from other babies in the Cook Children’s NICU.
Twins AmieLynn and JamieLynn Finley won the hearts of the nurses who fed, diapered and bathed the girls a little differently from other babies in the Cook Children’s NICU.
For the first three and a half months of their lives, AmieLynn and JamieLynn were joined from their breastbones to their bellies. The girls could lie only on their sides, face to face, because their chest/abdomen areas were connected. Caring for them in the NICU required some modification of the usual tools and techniques for infants.
Surgeons at Cook Children’s separated AmieLynn and JamieLynn on Jan. 23 in a rare and complex operation, a first for our medical center. Two separate isolettes brought the girls back to the NICU to recover under the watchful eye of the neonatologists and nurses who know them best.
“I’m excited that we’ve been part of their story,” said NICU Director Brittany McLaughlin, RN. “The team’s been very creative and innovative.”
Born in October at Texas Health Harris Methodist Hospital Fort Worth, the pair were transported at five weeks to Cook Children’s, where the NICU staff stepped up to the unique challenges of caring for conjoined twins. Consider diaper changes, for instance: “There’s lots of legs flailing everywhere. When they’re both awake and moving, you have to kind of wrangle one’s legs away while you change the other one,” said Brianne Galvan, RN. “You have to be fast.”
Or lifting their combined weight of about 22 pounds: “You’re not just picking up one heavy baby. It’s a lot more positioning,” said Raye Urbanek, RN. “You have double the number of wires you’re trying not to tangle as you’re taking them from the bed.”
Brianne has been JamieLynn’s primary nurse and Raye has been AmieLynn’s primary nurse since their arrival in November. NICU Manager Megan Maxwell, RN, prepared the setup for their room, which required a bit of layout reconfiguring for monitors and other equipment. Color coding – green for AmieLynn, purple for JamieLynn – designated the name bands, cords and other gear on each girl’s side of the bed.
 An additional step to safeguard patient identification happened every time the nurses turned the girls over. Nurses would alternate the spot where the girls’ heads and feet went in the bed to keep AmieLynn always on the left and JamieLynn always on the right after they were turned. “That’s so that we’re not confusing which one’s on which side,” Megan said. “That was obviously a big point of concern. We wanted to keep them safe.”
An additional step to safeguard patient identification happened every time the nurses turned the girls over. Nurses would alternate the spot where the girls’ heads and feet went in the bed to keep AmieLynn always on the left and JamieLynn always on the right after they were turned. “That’s so that we’re not confusing which one’s on which side,” Megan said. “That was obviously a big point of concern. We wanted to keep them safe.”
During the time they were conjoined, the girls’ faces were so close that they could suck on each other’s mouths. That made it tricky to feed them. Speech therapists at Cook Children’s helped by recommending ways to angle the twins’ heads to accommodate bottles.
Bath time required a round TurtleTub rather than the narrower standard model. The girls wore mittens even during their baths to cover their fingernails.
“We just swaddle them up and keep mittens on them because they will start to scratch on each other and then get angry,” Raye said. “If you keep the mittens on, then you can position them in the TurtleTub and have padding for their heads. They’re calm and happy and they love bath time.”
The twins could be propped up on a Boppy pillow or under a jungle gym for playtime. Other stimulation included music, physical and occupational therapy. Stretching exercises helped with the tight muscles in their necks and arms.
Family visits were key too. Their parents, James and Amanda, came to the NICU every day from Saginaw to feed and hold the girls. The babies liked to watch their entertaining 7-year-old brother and be soothed by the songs their grandmother sang to them.
Despite their shared anatomy, the twins developed distinct personalities. JamieLynn is known for her sass and strong will, while AmieLynn is easygoing and observant. Nurses say the girls used to arch their backs like they were trying to get away from each other. It wasn’t easy to keep a fussy baby from waking up her sleeping sister when they’re joined together.
“Amie’s gotten pretty good at sleeping through a lot of Jamie’s antics. But sometimes Jamie’s just punching her and it wakes her up and she is not happy,” Brianne said.
 The nurses use words like “amazing,” “feisty” and “beautiful” to describe the twins. They look forward to cuddling the girls one at a time. Now that they're recovering in separate beds, Brianne predicted that AmieLynn and JamieLynn would miss the constant close proximity of being connected. “We’re going to have to figure out something so they can see each other in the NICU.”
The nurses use words like “amazing,” “feisty” and “beautiful” to describe the twins. They look forward to cuddling the girls one at a time. Now that they're recovering in separate beds, Brianne predicted that AmieLynn and JamieLynn would miss the constant close proximity of being connected. “We’re going to have to figure out something so they can see each other in the NICU.”
Mary Frances Lynch, M.D. is the neonatologist for JamieLynn. Chad Barber, M.D. is the neonatologist for AmieLynn. Each has 16 years’ experience at Cook Children’s.
Dr. Lynch cited some medical complications that arose from conjoining:
- Limited mobility. The twins couldn’t be placed on their backs or tummies. They had to be turned frequently to prevent positional deformities and skin from breaking down.
- Breathing issues. JamieLynn needed oxygen by nasal cannula.
- Feeding concerns. IV nutrition and nasogastric feeding tubes allowed them to get their full feeding if they weren’t able to bottle feed. One twin grew significantly more than the other, likely related to their shared blood supply.
“Our primary focus in the NICU prior to surgery was to optimize their nutrition so that they could grow as much as possible,” Dr. Lynch said. “The bigger they are and the better their nutrition is, the easier their recovery after separation.”
During their post-surgery stay in the NICU, Dr. Barber said, major concerns include respiratory support and pain control. He and Dr. Lynch feel fortunate to take care of sick babies alongside the entire NICU team.
“It’s a big honor to be trusted by parents in the NICU,” Dr. Barber said. “Every day we have parents who are basically turning their child’s life over to us and believe in all the decisions that we make.”
About Cook Children's
Cook Children’s is more than a health care system: we strive to be an extension of your family, growing with your child from their first steps to adulthood. By collaborating to deliver on our Promise—to improve the well-being of every child in our care and our communities, we connect the dots for our patients. Between primary and specialty. Between home and medical home. Between short-term care and long-term health.
Based in Fort Worth, Texas, we’re 8,000+ dedicated team members strong, passionately caring for over 1.5 million patient encounters each year. Our integrated, not-for-profit organization spans two medical centers (including our new, state-of-the-art location in Prosper), two surgery centers, a physician network, home health services and a health plan. It also includes Child Study Center at Cook Children's, Cook Children's Health Services Inc., and Cook Children's Health Foundation.
And our impact extends beyond the borders of Texas. We proudly treat children from virtually every state in the nation and 32 countries. By seeing the world through the eyes of children and their families from all backgrounds, we’re able to shape health care suited to them: connected by kindness, imagination and respect — with an extra dose of magical wonder.
