Breathing Easier: Surgical Fix Expands Teen's Chest
Procedure raises the inward-growing sternum for patients with a sunken chest.
By Jean Yaeger
When Jack Coffey hit about age 13, the middle of his chest started to look dented in.
 And if he slouched a certain way, his insides felt cramped. Sometimes while skateboarding or playing the trumpet, Jack noticed a sharp pain from his breastbone pushing into his lungs. It didn’t take much exertion to run out of breath.
And if he slouched a certain way, his insides felt cramped. Sometimes while skateboarding or playing the trumpet, Jack noticed a sharp pain from his breastbone pushing into his lungs. It didn’t take much exertion to run out of breath.
The appearance of his caved-in chest also began to affect his confidence whenever he took off his shirt around friends.
“In the last couple years when it started getting more intense, I felt like I was getting a lot of looks,” he said. “It became almost a talking point conversation piece.”
His chest abnormality became more concerning when his pediatrician detected a possible heart murmur. Jack and his family were referred to Cook Children’s, where he underwent tests for a condition called pectus excavatum, also known as sunken-in chest.
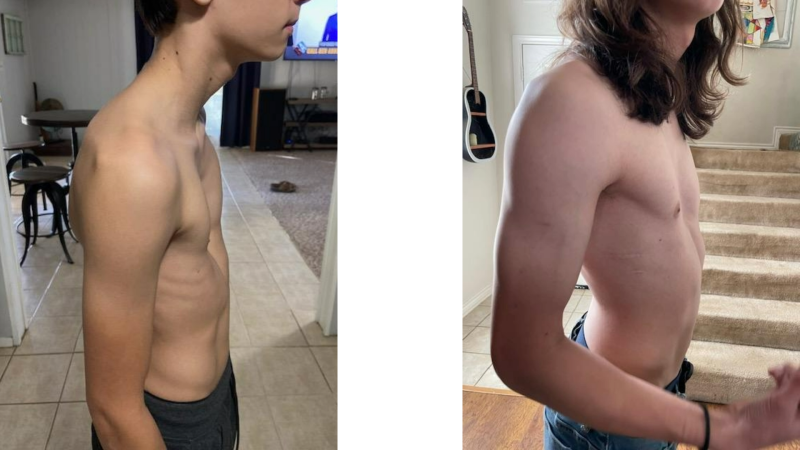
Pectus excavatum affects about 1 in 1,000 people whose sternum grows inward toward the spine. Cases can be mild, moderate or severe, as in Jack’s case. He thinks his scooped-out looking chest was about an inch and a half at its deepest point.
Jack chose to undergo surgery in December 2021 to correct the structure of his chest wall. Chad Hamner, M.D., a surgeon at Cook Children’s Medical Center – Fort Worth, inserted a curved metal bar that pushed up Jack’s sternum. It was a minimally invasive procedure with two small incisions and immediate results.
Jack was 15 at the time, and his first reaction afterward was to compare his fuller torso to a LEGO mini-figure.
“It’s almost like you changed out a LEGO piece. Like you put in a different middle body but kept the same legs and head,” said Jack, who’s now 17. “It felt strange, but instantly it felt like I had space to breathe.”
The bar stayed in place as his bones, joints and cartilage realigned and stabilized along the outward curve. Dr. Hamner monitored Jack at follow-up appointments over the next two years. In January 2024, the bar was removed during an outpatient procedure. Jack’s chest is less caved in now – and is expected to hold its shape.
Dr. Hamner monitored Jack at follow-up appointments over the next two years. In January 2024, the bar was removed during an outpatient procedure. Jack’s chest is less caved in now – and is expected to hold its shape.
Dr. Hamner estimated that surgeons at Cook Children’s do two or three dozen procedures for pectus excavatum each year. Severe cases like Jack’s can compress a child or teen’s heart and lungs, causing pain, shortness of breath or heart palpitations. Most people with the condition don’t have those symptoms, Dr. Hamner said.
The most common incentive for surgery is the desire to improve the appearance and self-esteem for adolescents who are self-conscious about their indented chest. Specialists at Cook Children’s can help you and your teen decide if and when surgery is the best option. Here’s what you need to know.
Diagnosis and Next Steps
People who have pectus excavatum were born with it, although it might not be noticed until the growth spurt of puberty. The cause isn’t always known, but there’s a higher risk for people with Marfan syndrome, a connective tissue disorder.
Dr. Hamner explained that the chest contains an intricate mesh of bones, joints and cartilage. If the sternum grows inward, and the ribs are protruding, the defect is more obvious. The name “excavatum” sounds like what it describes: a cave or cavity.
Children as young as 10 come to Cook Children’s to be checked out and possibly treated. Some patients tell Dr. Hamner they’ve eaten cereal out of their indentation or placed a baseball inside it.
“A lot of the time the kids are shy about it, and some of them don’t want to participate in activities or play sports if they have to change clothes in front of the other guys. They may be getting a little bit of bullying,” he said.
Patients who are considering surgery will first get a CT scan, which allows doctors to calculate how close the sternum has grown toward the spine. Candidates for surgery should be ideally nearing mid-puberty, around age 15, so that they’re mostly through growing by the time the bar comes out. The younger the patient is when the bar goes in, the longer the bar needs to remain in place.
“We tell families you have a range where the minimally invasive approach has a good result. And that’s typically until the time your cartilages become more rigid, up to your mid- to late 20s,” Dr. Hamner said. “A lot of the kids want to get it done before they’re dating, so they tend to want to do it earlier in adolescence.”
Dr. Hamner says many people choose to live with their sunken-in chest if it isn’t causing problems. He points out to his patients that pectus excavatum didn’t stop Olympic swimmer Cody Miller from excelling at his sport.
Inserting the Bar
When surgery is appropriate, doctors at Cook Children’s use the Nuss procedure. Dr. Hamner described these key points:
- Small incisions are made on each side of the chest. A camera and long-handled tool guide the surgical team as they make a path for a curved metal bar constructed of a nickel-titanium alloy.
- The bar is inserted in a U position. Once it’s under the sternum, the surgeon flips the bar, and the sternum raises up.
- A crossbar is sewn onto one side to help stabilize the hardware while the patient’s body adapts to its new shape over two to three years.
- Sometimes, two bars are needed to do the job.
Dr. Hamner compared the bars to the scaffolding that gives a building its form. How does it feel? It causes pressure and soreness, like when braces reposition your teeth. 
“If you stress a bone in a certain direction, it will remodel its shape in response to the stress,” he said. “In the Nuss procedure, you’re reshaping the chest wall by putting outward stress on the breastbone and ribs to break the bone down and rebuild it into a different shape. Ideally, when you take the bar out, the chest has reshaped itself to match the bar.”
To help with pain management, Cook Children’s uses a cryoablation device that numbs nerves along the chest wall. Cryoablation reduces the need for narcotics and other pain medications, and allows patients to go home from the hospital within two or three days of surgery, versus four or five days without cryoablation.
Patients can generally return to school within a week, Dr. Hamner said. They’re instructed to stand up straight and avoid contact sports for at least three months while their chest heals.
Complications from surgery are rare but can include allergy to the metal, infection, and puncture of the heart or heart sac. The pectus excavatum recurs less than 10% of the time.
Patient’s Perspective
Jack’s mom Audra Massoth said she first thought he might grow out his sunken-in chest when he got older and gained muscle mass. Instead of getting better, the pectus excavatum became more pronounced about the time he turned 13.
“Aside from the effects on his breathing, just cosmetically I didn’t want him to feel self-conscious taking his shirt off at pool parties or when we go to the lake,” she said. “That was probably the biggest thing for me. He is a super fit, super handsome kid. But I didn’t want him to feel like he wouldn’t be able to be comfortable taking his shirt off.”
They traveled to Fort Worth from their home in Azle for appointments with Dr. Hamner. Audra was in favor of surgery – but it was Jack’s decision, in the end.
Cryoablation reduced how much and how often Jack had to take medication to control the pain during recovery. His chest remained numb for a couple of months. Sleeping, meanwhile, was uncomfortable because the bar held his chest structure in place even when he turned onto his side.
Jack has two small scars on his sides – and he kept the bar and bracket as mementos of the two-year process of elevating his sternum. His heart murmur resolved itself because of the added room in his chest. He said he feels “evened out and straightened out” as he finishes high school, works as an electrician’s apprentice and pursues his passion for skateboarding.
Despite the painful recovery, Jack and his mom say they’re glad he went through the correction. He would tell other teens with pectus excavatum that he’s pleased with the results.
“The bar doesn’t stay forever. There’s good times and there’s bad times, but it’s 100% worth it.”
Experts in Pediatric Surgery
When your child requires surgery, you want to be certain you receive the most advanced care possible from the most experienced medical team. The surgeons at Cook Children's specialize in pediatric procedures from the simplest to the most complex, including congenital malformations, head and neck masses, abdominal issues and tumors. You can trust that our specialists understand the very specific needs of a child before, during and after surgery. Visit us here to find a map and learn about appointments, referrals and more.
RELATED STORY:
Get to know Chad Hamner, M.D.
 An Alabama native, Dr. Hamner moved to Fort Worth in 2009 when he came to Cook Children's Medical Center. He serves as the Medical Director for Pediatric Trauma Services and Surgical Director of Pediatric Critical Care Services. He is a Fellow of the American College of Surgeons and is board certified in Pediatric Surgery, Surgical Critical Care, and General Surgery. He completed training in General Surgery at the Mayo Clinic, Rochester MN, Surgical Critical Care at Nationwide Children’s Hospital in Columbus, OH, and Pediatric Surgery at Cohen Family Children’s Medical Center in New Hyde Park, NY. He is an Assistant Professor in the Division of Surgery for Texas Christian Burnett School of Medicine. His clinical interests include trauma, critical care of neonates and children, congenital anomalies, tumors and chest wall deformities. When Dr. Hamner’s not in surgery, he enjoys spending time with his wife, coaching their four sons in sports, traveling, working in carpentry and cheering on the Alabama Crimson Tide.
An Alabama native, Dr. Hamner moved to Fort Worth in 2009 when he came to Cook Children's Medical Center. He serves as the Medical Director for Pediatric Trauma Services and Surgical Director of Pediatric Critical Care Services. He is a Fellow of the American College of Surgeons and is board certified in Pediatric Surgery, Surgical Critical Care, and General Surgery. He completed training in General Surgery at the Mayo Clinic, Rochester MN, Surgical Critical Care at Nationwide Children’s Hospital in Columbus, OH, and Pediatric Surgery at Cohen Family Children’s Medical Center in New Hyde Park, NY. He is an Assistant Professor in the Division of Surgery for Texas Christian Burnett School of Medicine. His clinical interests include trauma, critical care of neonates and children, congenital anomalies, tumors and chest wall deformities. When Dr. Hamner’s not in surgery, he enjoys spending time with his wife, coaching their four sons in sports, traveling, working in carpentry and cheering on the Alabama Crimson Tide.
